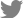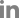Case Report
A 60-year-old male suffering from back pain radiating to lower extremities bilaterally and gait disturbance for the past 6 months visited our out-patient department. Physical examination revealed hypoesthesia, decreased perception of pain, temperature, and fine touch below the level of T6, and difficulty in voiding. Muscle strength was 5/5 according to the medical research council grading system in all the muscle groups. He had a normal body mass index (BMI), and past clinical and family history were unremarkable.
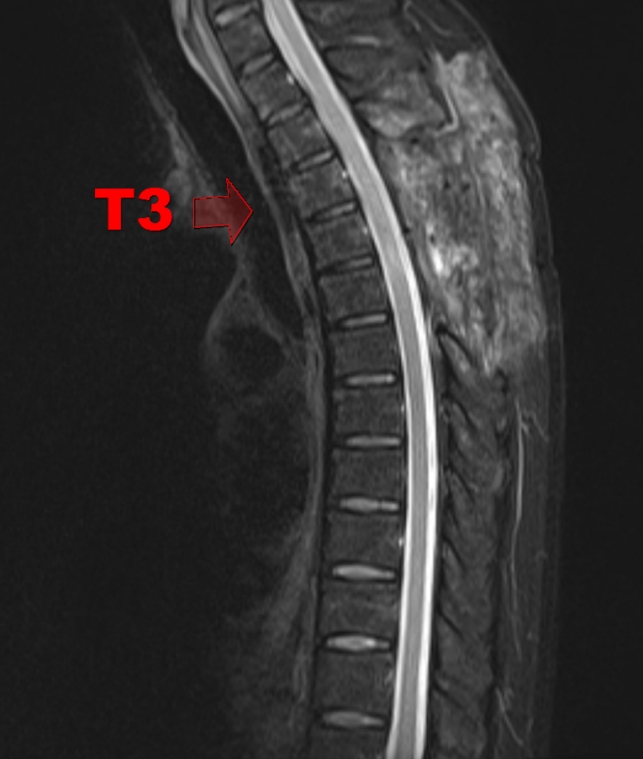
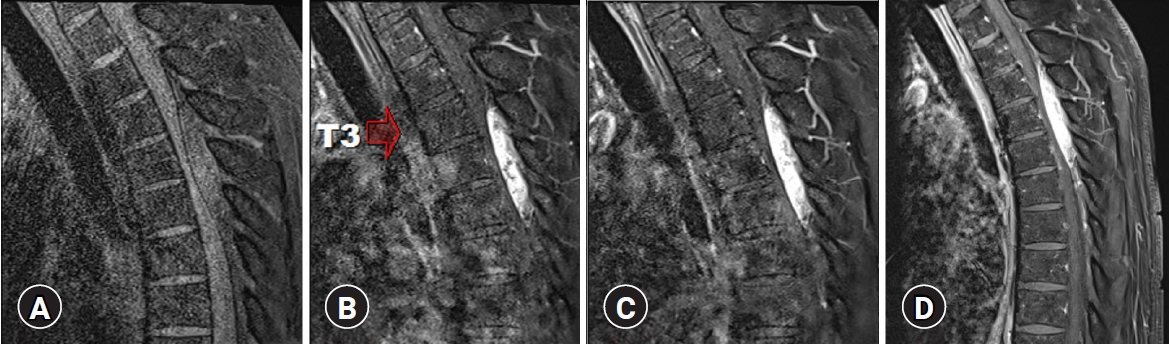
Sagittal T1-weighted MRI showed a lenticular-shaped mass, 5.7 cm in size, at the T3-T5 posterior epidural space with heterogeneous iso-intensity to low-intensity relative to the spinal cord (
Fig. 1A). Sagittal T2-weighted MRI showed a high-intensity lesion (
Fig. 1B), whereas sagittal T1 post-contrast MRI showed persistent hyperenhancement (
Fig. 1C). Based on these findings, epidural hematoma was first suspected. DCE-MRI was performed afterwards, and its findings pointed toward the presence of a meningioma or angiolipoma.
Total surgical resection of the mass was planned. We performed total laminectomy at the level of T3 to T5 with gross total resection. A large firm highly vascular yellowish-brown mass receiving blood supply from many epidural vessels was found with a small hematoma at the T3-T5 posterior epidural space. The yellowish fat layer was clearly demarcated from the dura. The epidural vessels appeared to arise from the lateral side. During tumor resection, a large amount of bleeding occurred; therefore, piecemeal removal was performed. In addition, no infiltration of bone or surrounding tissues was observed (
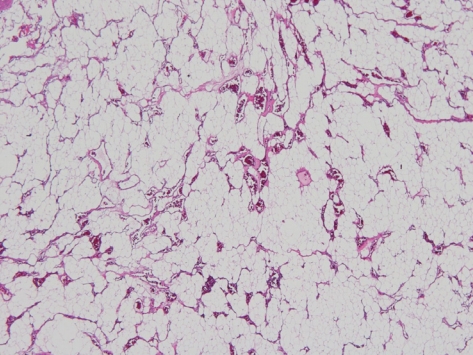
Fig. 2). Neurophysiological monitoring was performed during the operation and no specific findings were seen. Pathological analysis of frozen biopsy measuring 1.4 ├Ś 1.0 cm in size showed mature and immature fatty tissue measuring 1.4 g in weight, whereas analysis of the biopsy measuring 2.6 ├Ś 2.1 ├Ś 0.3 cm in size revealed the presence of fat and capillary-sized vessels, which confirmed the diagnosis of angiolipoma (
Fig. 3).
The patientŌĆÖs symptoms improved after the operation. However, antibiotics were administered for 16 days due to high C-reactive protein (CRP) levels and the patient was discharged after the discontinuation of antibiotics when the CRP level returned to normal. Three months after the operation, MRI follow-up was performed and there was no recurrence (
Fig. 4).
This study was approved by the Institutional Review Board of Pusan National University Yangsan Hospital (IRB No: 05-2021-110). Written informed consent by the patients was waived due to a retrospective nature of our study.
Discussion
The basic etiology of angiolipoma has not been elucidated yet [
6]. It is a disease that mainly occurs in the subcutaneous tissue of the trunk and limbs. It rarely involves the spinal cord, and occurs mainly on the dorsal aspect of the thoracic levels. However, some studies have suggested that angiolipoma develops as a result of pluripotent mesenchymal stem cells with secretory activity, and malignant transformation and involvement of neural tissue has not yet been reported [
7]. Angiolipoma occurs predominantly in women and obese people, and is more likely to be observed in pregnant women with sudden weight gain [
8]. Pregnancy interferes with spinal venous drainage and increases epidural venous pressure. In addition, adiposity increases due to the hormonal effects of pregnancy, which may lead to the proliferation of angiolipoma [
9].
Extradural spinal angiolipoma was first observed on autopsy in 1890. Pathological reports were first published by Howard in 1960 [
7]. Pathological features include fat and vessels in a ratio of 1:3 to 2:3 and consist of mature fat cells, and abnormal capillary, sinusoidal, venous, or arterial vascular tissues [
10]. Pathologically, lesions with copious smooth muscle proliferation are subclassified as angiomyolipoma [
11]. The tumor resected in the present case was composed of adipocyte and capillary-sized vessels. It was not significantly different from other angiolipomas (
Fig. 3).
Plain radiography is the most basic investigation that can be performed initially; but its ability to detect the tumors is limited. However, infiltrating tumors may show erosion of the pedicle, widening of the spinal canal, and trabeculation of the vertebral body on X-ray [
11,
12]. There was no abnormal X-ray finding in the present case.
On computed tomography (CT), spinal angiolipoma generally shows low or intermediate-density. On contrast-enhanced CT, angiolipoma appears hypodense, whereas some tumors have an isodense appearance, which is related to the rich and extensive vascularity [
13]. In this case, CT scan showed a lenticular shaped mass with heterogeneous isodensity at T3-T5 posterior epidural space.
MRI is the gold standard for the diagnosis of spinal angiolipoma [
14]. Spinal angiolipoma usually appears homogenous and hypointense on T1-weighted images due to the fat content. On T2-weighted images, it can show a variable pattern, but it is mostly hyperintense. In this case, heterogeneous, iso and low-intensity signals were seen on MRI T1-weighted images and heterogeneous and high-intensity signals were seen on T2-weighted images. Therefore, hematoma was suspected. An additional investigation (DCE-MRI) was also performed. Gadolinium is injected in DCE-MRI to obtain vascularization and perfusion data by analyzing the tissue changes. This is useful for the diagnosis and treatment of the brain and breast tumors. When DCE-MRI of the spine is performed, the vascularity, perfusion, and capillary permeability of the tumor can be analyzed [
15,
16]. In this case, DCE-MRI showed high vascularity with early and persistent hyperenhancement of the tumor (
Fig. 5). Angiography can also be used for the diagnosis and treatment of some spinal angiolipomas. Resection of a highly vascularized spinal angiolipoma that appears hypointense on the T1-weighted images may be facilitated by embolization before surgery [
10].
Symptoms of spinal angiolipoma vary according to the tumor location and its compression of the surrounding structures. Most sensory and motor deficits occur below the level of the lesion, which is similar to the symptoms of spinal cord compression. Spinal angiolipoma is characterized by slow progression, enlarging gradually over months, with diagnoses occurring within a year [
17,
18]. The occurrence of symptoms may be due to poor vascular drainage, which may lead to engorgement, enlargement or degeneration of the blood vessels. The occurrence of steal phenomenon, venous thrombosis, and hemorrhage can contribute to the development or sudden worsening of the symptoms [
17,
19,
20]. Only a few cases have been reported in which hemorrhagic transformation of angiolipoma was accompanied by the sudden exacerbation of the neurological symptoms. Akhaddar et al. [
3] reported the first such case in 2008. This was a case of a 47-year-old male who developed sudden paresthesia and complete neurological palsy within a few minutes due to the hemorrhagic epidural angiolipoma. In 2018 Horiuchi et al. [
4] reported the case of a 49-year-old female with obesity (BMI, 31.1 kg/m
2) who presented with a 1-week history of progressively worsening back pain, paresthesia of the lower limbs, and gait disturbance. Surgery was performed and angiolipoma was diagnosed on the pathological examination after surgery. In 2020, an unusual case was reported in angiolipoma underwent hemorrhagic transformation due to a traumatic factor (back massage) [
5]. In this case, DCE-MRI was used to make the diagnosis of a mass, rather than simple hematoma, before surgery. The diagnosis of a tumor should not be missed because of the presence of hemorrhage. DCE-MRI before and pathological analysis during surgery must be performed for the diagnosis.
Spinal angiolipoma is classified into two types, non-infiltrating and infiltrating. The non-infiltrating type is more common and exhibits encapsulation. However, the infiltrating type has indefinite boundaries, is mainly unencapsulated, has sporadic features, and occasionally shows infiltration of the bone and surrounding tissues. Although there is some difference in the treatment plan, surgical resection is the gold standard regardless of the type. Total tumor resection is the treatment of choice, but it may be difficult to achieve for the infiltrating type. Even with subtotal removal, most patients show good results. This is due to the nature of the tumor, because it does not undergo malignant transformation and is slow-growing. In addition, in the case of recurrent tumor as reported by Gonzalez-Crussi et al. [
13], combined treatment with radiotherapy and surgery may be performed. In case of highly vascularized spinal angiolipoma, embolization is performed before attempting surgical removal [
10].
The mean age of incidence of spinal angiolipoma is 42.9 years (range, 10 days-85 years). The incidence of spinal angiolipoma is expected to increase in the aging societies. Comorbid conditions need to be considered before performing surgery in elderly patients. However, spinal angiolipoma surgery has good outcomes. Even though, caution should be exercised in the treatment of elderly patients with spinal angiolipoma, surgical resection remains the recommended treatment for these patients.












 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print